ASTM F3142-16
(Guide)Standard Guide for Evaluation of in vitro Release of Biomolecules from Biomaterials Scaffolds for TEMPs
Standard Guide for Evaluation of <emph type="bdit">in vitro</emph> Release of Biomolecules from Biomaterials Scaffolds for TEMPs
SIGNIFICANCE AND USE
4.1 The European Pharmacopoeia (Ph. Eur.) as well as the United States Pharmacopeia (USP) describe several dissolution and drug release setups for tablets, capsules, transdermal patches and suppositories (USP , USP , Ph. Eur. 2.9.3, Ph. Eur. 2.9.4). However, up to this point no pharmacopoeia standardized in-vitro release test has been established for parenteral dosage forms which provide sustained drug release, for example, implants.
4.2 An appropriately designed in-vitro release test would be favorable in the early stage of development of biomolecule-releasing scaffolds for TEMPs, as well as in quality control, and may help to reduce the number of animal experiments.
4.3 Appendix X1 provides a tabulated overview of published in-vitro release studies performed with biomaterial scaffolds loaded with biomolecules.
4.4 One goal of in-vitro release studies is to simulate the in-vivo conditions as closely as possible, but with sufficiently simplifying abstraction. The simplification comprises two general aspects: the amount of fluid or release medium in contact with the implant to simulate the physiological environment, and the composition of that release medium.
SCOPE
1.1 To describe general principles of developing and/or using an in vitro assay to evaluate biomolecule release from biomaterials scaffolds for TEMPs, with examples from the literature
1.2 The guide will address scaffolds that do not contain seeded cells; general principles may still apply but may need to be modified if cells are part of the TEMPs.
1.3 In vitro release assessment of biomolecules from matrices is a valuable tool for screening biomolecule-scaffold interactions, as well as characterization, and/or quality control.
1.4 The values stated in SI units are to be regarded as standard. No other units of measurement are included in this standard.
1.5 This standard does not purport to address all of the safety concerns, if any, associated with its use. It is the responsibility of the user of this standard to establish appropriate safety and health practices and determine the applicability of regulatory limitations prior to use.
General Information
- Status
- Published
- Publication Date
- 14-Nov-2016
- Technical Committee
- F04 - Medical and Surgical Materials and Devices
- Drafting Committee
- F04.42 - Biomaterials and Biomolecules for TEMPs
Relations
- Effective Date
- 01-Feb-2020
- Effective Date
- 01-Dec-2016
- Effective Date
- 01-Dec-2016
- Effective Date
- 01-Dec-2012
- Effective Date
- 01-Apr-2011
- Effective Date
- 15-Aug-2010
- Effective Date
- 01-Jun-2010
- Effective Date
- 01-Nov-2004
- Effective Date
- 10-Sep-2003
- Referred By
ASTM F3354-19 - Standard Guide for Evaluating Extracellular Matrix Decellularization Processes - Effective Date
- 15-Nov-2016
- Effective Date
- 15-Nov-2016
Overview
ASTM F3142-16: Standard Guide for Evaluation of in vitro Release of Biomolecules from Biomaterials Scaffolds for TEMPs is a globally recognized standard developed by ASTM International. This guide provides comprehensive principles and considerations for developing, validating, and using in vitro release assays to evaluate the controlled release of biomolecules from biomaterial scaffolds, particularly those used in Tissue Engineered Medical Products (TEMPs). As there is no harmonized pharmacopoeial test for sustained-release parenteral dosage forms (for example, implants), ASTM F3142-16 fills an important gap for researchers, developers, and quality control professionals working in the field of biomaterials and drug delivery.
Key Topics
- Scope and Application: The guide applies to in vitro release evaluation of biomolecules from scaffolds without cell seeding, with adaptable principles for cell-containing products.
- In vitro Release Assay Design:
- Addresses essential factors including sample preparation, medium selection, vessel design, and temperature control.
- Focuses on simulating physiological environments, considering osmolality, pH, and relevant medium additives (e.g., PBS, BSA, FBS).
- Methodological Considerations:
- Discusses both static and dynamic (flow-through) conditions to best mimic in vivo performance.
- Emphasizes selecting appropriate analytical techniques (e.g., ELISA, HPLC, UV spectroscopy) for quantifying biomolecule release.
- Quality Control and Characterization:
- Highlights the value of in vitro release studies in early product development, scaffold-biomolecule interaction screening, and lot-to-lot consistency.
- Promotes reducing animal testing by providing reliable in vitro methods.
- Interference and Validation:
- Addresses potential interferences from proteinaceous media and scaffold materials.
- Stresses the importance of validating analytical assays under specific experimental conditions, including sensitivity, specificity, and stability considerations.
Applications
- Product Development for TEMPs: This standard is vital for pharmaceutical and biomedical industries developing biomolecule-loaded scaffolds for controlled drug delivery and regenerative medicine.
- Regulatory Submission and Compliance: Applies to the generation of data for regulatory filings, ensuring consistency and reliability in in vitro drug release data.
- Quality Assurance and Control: Provides methodologies for batch release testing and post-market monitoring of biomaterial-based products.
- Research and Academia: Offers a reference framework for academic investigators designing studies on drug release kinetics and biomaterials interaction.
- Reduction of Animal Experiments: Supports ethical research by enabling robust in vitro screening before in vivo evaluation.
Related Standards
ASTM F3142-16 is designed in alignment with and often used alongside several national and international standards, including:
- ASTM Standards:
- F2312 - Terminology Relating to Tissue Engineered Medical Products
- F2809 - Terminology for Medical and Surgical Materials and Devices
- F2902 - Guide for Assessment of Absorbable Polymeric Implants
- United States Pharmacopeia (USP):
- USP <711>: Dissolution
- USP <724>: Drug Release
- USP <785>: Osmolality/Osmolarity
- USP <1092>: Dissolution Procedure Development and Validation
- USP <1>: Parenteral Product Quality Tests
- European Pharmacopoeia (Ph. Eur.):
- 2.9.3: Dissolution Test for Solid Dosage Forms
- 2.9.4: Dissolution Test for Transdermal Patches
- 2.9.25: Dissolution Test for Medicated Chewing Gums
- FDA Guidance: Bioanalytical Method Validation
Practical Value
ASTM F3142-16 is a fundamental standard for anyone involved in the design, development, and quality control of biomaterial-based sustained-release systems. By establishing clear guidelines for in vitro release testing, it enhances product reliability, regulatory acceptance, and supports ethical research practices. For manufacturers and laboratories, adoption of ASTM F3142-16 leads to improved reproducibility, robust data for regulatory review, and more efficient product development pathways in the rapidly evolving fields of biomaterials and tissue engineering.
Buy Documents
ASTM F3142-16 - Standard Guide for Evaluation of <emph type="bdit">in vitro</emph> Release of Biomolecules from Biomaterials Scaffolds for TEMPs
Get Certified
Connect with accredited certification bodies for this standard

BSI Group
BSI (British Standards Institution) is the business standards company that helps organizations make excellence a habit.

TÜV Rheinland
TÜV Rheinland is a leading international provider of technical services.

TÜV SÜD
TÜV SÜD is a trusted partner of choice for safety, security and sustainability solutions.
Sponsored listings
Frequently Asked Questions
ASTM F3142-16 is a guide published by ASTM International. Its full title is "Standard Guide for Evaluation of <emph type="bdit">in vitro</emph> Release of Biomolecules from Biomaterials Scaffolds for TEMPs". This standard covers: SIGNIFICANCE AND USE 4.1 The European Pharmacopoeia (Ph. Eur.) as well as the United States Pharmacopeia (USP) describe several dissolution and drug release setups for tablets, capsules, transdermal patches and suppositories (USP , USP , Ph. Eur. 2.9.3, Ph. Eur. 2.9.4). However, up to this point no pharmacopoeia standardized in-vitro release test has been established for parenteral dosage forms which provide sustained drug release, for example, implants. 4.2 An appropriately designed in-vitro release test would be favorable in the early stage of development of biomolecule-releasing scaffolds for TEMPs, as well as in quality control, and may help to reduce the number of animal experiments. 4.3 Appendix X1 provides a tabulated overview of published in-vitro release studies performed with biomaterial scaffolds loaded with biomolecules. 4.4 One goal of in-vitro release studies is to simulate the in-vivo conditions as closely as possible, but with sufficiently simplifying abstraction. The simplification comprises two general aspects: the amount of fluid or release medium in contact with the implant to simulate the physiological environment, and the composition of that release medium. SCOPE 1.1 To describe general principles of developing and/or using an in vitro assay to evaluate biomolecule release from biomaterials scaffolds for TEMPs, with examples from the literature 1.2 The guide will address scaffolds that do not contain seeded cells; general principles may still apply but may need to be modified if cells are part of the TEMPs. 1.3 In vitro release assessment of biomolecules from matrices is a valuable tool for screening biomolecule-scaffold interactions, as well as characterization, and/or quality control. 1.4 The values stated in SI units are to be regarded as standard. No other units of measurement are included in this standard. 1.5 This standard does not purport to address all of the safety concerns, if any, associated with its use. It is the responsibility of the user of this standard to establish appropriate safety and health practices and determine the applicability of regulatory limitations prior to use.
SIGNIFICANCE AND USE 4.1 The European Pharmacopoeia (Ph. Eur.) as well as the United States Pharmacopeia (USP) describe several dissolution and drug release setups for tablets, capsules, transdermal patches and suppositories (USP , USP , Ph. Eur. 2.9.3, Ph. Eur. 2.9.4). However, up to this point no pharmacopoeia standardized in-vitro release test has been established for parenteral dosage forms which provide sustained drug release, for example, implants. 4.2 An appropriately designed in-vitro release test would be favorable in the early stage of development of biomolecule-releasing scaffolds for TEMPs, as well as in quality control, and may help to reduce the number of animal experiments. 4.3 Appendix X1 provides a tabulated overview of published in-vitro release studies performed with biomaterial scaffolds loaded with biomolecules. 4.4 One goal of in-vitro release studies is to simulate the in-vivo conditions as closely as possible, but with sufficiently simplifying abstraction. The simplification comprises two general aspects: the amount of fluid or release medium in contact with the implant to simulate the physiological environment, and the composition of that release medium. SCOPE 1.1 To describe general principles of developing and/or using an in vitro assay to evaluate biomolecule release from biomaterials scaffolds for TEMPs, with examples from the literature 1.2 The guide will address scaffolds that do not contain seeded cells; general principles may still apply but may need to be modified if cells are part of the TEMPs. 1.3 In vitro release assessment of biomolecules from matrices is a valuable tool for screening biomolecule-scaffold interactions, as well as characterization, and/or quality control. 1.4 The values stated in SI units are to be regarded as standard. No other units of measurement are included in this standard. 1.5 This standard does not purport to address all of the safety concerns, if any, associated with its use. It is the responsibility of the user of this standard to establish appropriate safety and health practices and determine the applicability of regulatory limitations prior to use.
ASTM F3142-16 is classified under the following ICS (International Classification for Standards) categories: 11.100.10 - In vitro diagnostic test systems. The ICS classification helps identify the subject area and facilitates finding related standards.
ASTM F3142-16 has the following relationships with other standards: It is inter standard links to ASTM F2312-11(2020), ASTM F2902-16e1, ASTM F2902-16, ASTM F2902-12, ASTM F2312-11, ASTM F2809-10, ASTM F2312-10, ASTM F2312-04, ASTM F2312-03, ASTM F3354-19, ASTM F3510-21. Understanding these relationships helps ensure you are using the most current and applicable version of the standard.
ASTM F3142-16 is available in PDF format for immediate download after purchase. The document can be added to your cart and obtained through the secure checkout process. Digital delivery ensures instant access to the complete standard document.
Standards Content (Sample)
This international standard was developed in accordance with internationally recognized principles on standardization established in the Decision on Principles for the
Development of International Standards, Guides and Recommendations issued by the World Trade Organization Technical Barriers to Trade (TBT) Committee.
Designation: F3142 − 16
Standard Guide for
Evaluation of in vitro Release of Biomolecules from
Biomaterials Scaffolds for TEMPs
This standard is issued under the fixed designation F3142; the number immediately following the designation indicates the year of
original adoption or, in the case of revision, the year of last revision. A number in parentheses indicates the year of last reapproval. A
superscript epsilon (´) indicates an editorial change since the last revision or reapproval.
1. Scope USP <711> Dissolution
USP <724> Drug Release
1.1 To describe general principles of developing and/or
USP <785> Osmolality and Osmolarity
using an in vitro assay to evaluate biomolecule release from
USP <1092> The Dissolution Procedure: Development and
biomaterials scaffolds for TEMPs, with examples from the
Validation
literature
2.3 European Pharmacopeia (Ph. Eur.):
1.2 The guide will address scaffolds that do not contain
Ph. Eur. 2.9.3 Dissolution Test for Solid Dosage Forms
seededcells;generalprinciplesmaystillapplybutmayneedto
Ph. Eur. 2.9.4 Dissolution Test for Transdermal Patches
be modified if cells are part of the TEMPs.
Ph. Eur. 2.9.25 Dissolution Test for Medicated Chewing
1.3 In vitro release assessment of biomolecules from matri- Gums
ces is a valuable tool for screening biomolecule-scaffold
2.4 FDA Document:
interactions, as well as characterization, and/or quality control. FDAGuidanceforIndustry BioanalyticalMethodValidation
(2001)
1.4 The values stated in SI units are to be regarded as
standard. No other units of measurement are included in this
3. Terminology
standard.
3.1 ThepresentdocumentusesthedefinitionsofTerminolo-
1.5 This standard does not purport to address all of the
gies F2809 and F2312.
safety concerns, if any, associated with its use. It is the
responsibility of the user of this standard to establish appro-
4. Significance and Use
priate safety and health practices and determine the applica-
4.1 The European Pharmacopoeia (Ph. Eur.) as well as the
bility of regulatory limitations prior to use.
UnitedStatesPharmacopeia(USP)describeseveraldissolution
and drug release setups for tablets, capsules, transdermal
2. Referenced Documents
patches and suppositories (USP <711>, USP <724>, Ph. Eur.
2.1 ASTM Standards:
2.9.3, Ph. Eur. 2.9.4). However, up to this point no pharmaco-
F2312 Terminology Relating to Tissue Engineered Medical
poeia standardized in-vitro release test has been established for
Products
parenteral dosage forms which provide sustained drug release,
F2809 Terminology Relating to Medical and Surgical Mate-
for example, implants.
rials and Devices
4.2 An appropriately designed in-vitro release test would be
F2902 Guide for Assessment of Absorbable Polymeric Im-
favorable in the early stage of development of biomolecule-
plants
releasing scaffolds for TEMPs, as well as in quality control,
2.2 United States Pharmacopeia (USP) General Chapters:
and may help to reduce the number of animal experiments.
USP<1> Injections and Implanted Drug Products
(Parenterals)—Product Quality Tests
4.3 Appendix X1 provides a tabulated overview of pub-
lished in-vitro release studies performed with biomaterial
scaffolds loaded with biomolecules.
This test method is under the jurisdiction ofASTM Committee F04 on Medical
and Surgical Materials and Devices and is the direct responsibility of Subcommittee
4.4 One goal of in-vitro release studies is to simulate the
F04.42 on Biomaterials and Biomolecules for TEMPs.
in-vivo conditions as closely as possible, but with sufficiently
Current edition approved Nov. 15, 2016. Published January 2017. DOI: 10.1520/
F3142-16.
For referenced ASTM standards, visit the ASTM website, www.astm.org, or
contact ASTM Customer Service at service@astm.org. For Annual Book of ASTM Available from EDQM Council of Europe, 7 allée Kastner, CS 30026, F-67081
Standards volume information, refer to the standard’s Document Summary page on Strasbourg, France, or visit the website, www.edqm.eu.
the ASTM website. Available from Drug Information Branch (HDF-210), Center for Drug Evalu-
Available from U.S. Pharmacopeial Convention (USP), 12601 Twinbrook ation and Research (CDER), 5600 Fishers Lane, Rockville, MD 20857, or visit the
Pkwy., Rockville, MD 20852-1790, http://www.usp.org. website, http://www.fda.gov/cder/guidance/index.
Copyright © ASTM International, 100 Barr Harbor Drive, PO Box C700, West Conshohocken, PA 19428-2959. United States
F3142 − 16
simplifying abstraction. The simplification comprises two gen- 5.2.4 One of the important factors is to determine if there
eral aspects: the amount of fluid or release medium in contact are any solubility issues for the biomolecule, in order to define
with the implant to simulate the physiological environment, the most appropriate medium. This primary evaluation can be
and the composition of that release medium. achieved by exposing the biomolecule to the same experimen-
tal conditions without the scaffold present, to create a baseline
5. Elements of in vitro Release Assays in the candidate medium, and comparing it to a known stable
formulation of the biomolecule at the same concentration
5.1 Sample (biomaterial scaffold loaded with biomo-
levels. If the concentrations measured in the candidate medium
ecule(s)):
are substantially the same as in the known stable formulation,
5.1.1 The sample should be taken from the final product,
it is a good indicator for sufficient solubility and minimum
manufactured by a representative process including packaging
absorption to surfaces in the system (see also 5.3.5).
and sterilization.
5.2.5 If the experiment is set up for an extended period of
5.1.2 Thereareseveralconsiderationsthatwillinfluencethe
time to simulate the target period of release in vivo (that is,
selection of the sample dimensions.
several days to weeks or months), consider adding azides or
5.1.2.1 Vessel size into which the sample can physically fit.
other preservatives to maintain the sterility of the medium and
5.1.2.2 Method used to generate a representative sample,
aseptic conditions in the setup. Possible impact of any additive
where needed, for example, by biopsy punch, cutting with a
on either the sample or the analytical method should be
scalpel blade.
evaluated.
5.1.2.3 Load of the biomolecule, and the concentration in
5.2.6 The ratio of the volume of release medium to biomol-
the final setup.
ecule load (which may correspond to the volume or size of the
construct) is important. If there is a requirement to have sink
5.2 Release Medium:
conditions in the experiment (for example, to simulate implan-
5.2.1 In order to simulate physiologic conditions at the
tation sites with high fluid circulation), then sink conditions
intended implant site, the release medium should be of appro-
can be achieved by using a large volume of release medium at
priate tonicity (osmolality) and pH. Regarding osmolality, the
the beginning of the experiment and extraction of small
term is used according to USP<785> and as such is a measure
aliquots, or frequent exchange of the medium. Per USP
of concentration of real solutes, expressed in osmole per [kg]
definition, sink conditions can be maintained at about three
of soluent. Isotonic solutions are iso-osmotic relative to whole
times the volume of a saturated solution, and it has been
blood. Isotonicity is a target attribute for parenteral injections
suggested that it should remain below 10 % of saturation
per USP <1>.
concentration in the solution (Reference: USP <1092>). As
NOTE 1—Cells, for example red blood cells, are susceptible to condi-
indicated in 5.2.4, and 5.8.8, the saturation concentration in the
tions that are outside the isotonic range, by showing swelling through
candidate medium may need to be experimentally determined.
influx of water through the cell membrane (potentially leading to burst)
when in a hypotonic environment, or shrinking through efflux of water
NOTE 2—Solubility of biomolecules is dependent on pH, salts, and
through the cell membrane when in a hypertonic environment. Regarding
temperature,andmayvarywidelynotonlybetweenbiomoleculesbutalso
pH, the medium should be buffered to prevent pH shifts over time due to
foreachbiomoleculeatdifferentconditions(forexample,BSAreportedto
the release of the biomolecule, and/or degradation of the matrix. pH shifts
be soluble in water at 40 mg/mL; vendor data sheets for basic fibroblast
could change the release mechanism or kinetics.
growth factor (bFGF), nerve growth factor (NGF), and bone morphoge-
neticprotein-2(BMP-2)recommendreconstitutionoflyophilizedmaterial
5.2.2 One medium used very often in the published litera-
to not less than 100ug/mL. Note that lyophilized material is typically
ture is phosphate-buffered saline (PBS), pH 7.2 or 7.4, in the
formulated and contains some buffer/salt/stabilizers).
range of isotonicity (approximately 300 mOsm/kg). In this
5.2.7 The addition of a protease or other enzyme may be
case, the buffer system is provided by phosphate salts; the
considered, if the biomolecule is expected to be tightly bound
tonicity is typically augmented with sodium chloride.
or incorporated. The presence of the protease or other enzyme
5.2.3 The release medium may be spiked with other com-
may interfere with the assay used to quantify the biomolecule
ponents to make it more similar to serum, for example, bovine
of interest (see 5.2.3). Also, the susceptibility of the biomol-
serum albumin (BSA), or fetal bovine serum (FBS; multicom-
ecule of interest to the protease or other enzyme must be
ponent additive). It should be noted that these additives can
experimentally evaluated.
substantially interfere with the detection method (see 5.7). If
5.2.8 5.2.8 In cases where the biomolecule is tightly bound
protein components are added to the medium (BSA, FBS),
or incorporated, harsher extraction media may be required. For
evaluation of in vitro release will require more specific and/or
example, for extraction of BMP-2 from bone matrix, buffers
sophisticated assays (compared to simple A280 UV detection
containing urea (Urist 1984 (1)) , ethylene glycol (Urist 1979
for concentration), as both the biomolecule that is studied, and
(2)), or an arginine-histidine combination (Hollinger 1996 (3))
the proteinaceous component(s) of the medium may contribute
have been described.
to the detected signal. The same applies if there are several
5.3 Vessel/Container:
biomolecules that can be released from the biomaterial scaf-
fold. Further considerations are described in 5.8 (especially 5.3.1 The vessel needs to be of appropriate size to contain
the sample as well as the medium.
5.8.4 and 5.8.6). It should also be noted that regarding the use
of BSA and FBS, it is important to limit the use to a single or
limitednumberoflotstoreducevariabilityintheassaysystem,
The boldface numbers in parentheses refer to a list of references at the end of
especially for studies that require more than a single iteration. this standard.
F3142 − 16
5.3.2 The vessel needs to have a tight closure, and tight from the construct to avoid accidentally removing parts of the
connections in any fluid paths, to keep the system intact. The construct. Alternatively, separation of the releasing construct
main concerns are microbiological contamination, but also from the bulk of the medium has been achieved by placing the
evaporation which could impact concentration. construct inside a dialysis membrane, or reverse dialysis
5.3.3 USP <711> and USP <724> describe several vessel (construct in the bulk of the medium, samples pulled from the
configurations that may be appropriate and commercially dialysis cassette).
available to evaluate in vitro release of biomolecules from 5.6.3 Options include manual sampling, or automation.
biomaterials scaffolds for TEMPs. Automation may decrease the risk of accidental contamination
during sample pull, as well as operator errors (for example,
5.3.4 Vessels may be flow-through cells, or static vessels
with internal, external, or no mixing mechanism. Mixing pulled versus replaced volume, timing, etc.). Some setups may
offer the option of in-line measurements in a circulating
versus static conditions are discussed further in 5.5.
system.
5.3.5 The surface and contact materials should be evaluated
regarding adsorption or absorption characteristics of the
5.7 Sampling Time Points and Total Time:
biomolecule at the concentrations expected in the experiment.
5.7.1 The frequency of sampling can influence the release
Adsorption/absorption phenomena could have an effect on
by creating sink conditions versus no-sink conditions. As
concentration results, as well as the structural integrity of the
mentioned above, sink conditions are maintained when the
molecule.
volume exceeds approximately three times the saturation
concentration. Frequent sampling (with replenishing), or sam-
5.4 Temperature-Controlled Environment:
pling a large amount of the medium at a lower frequency, is
5.4.1 The experimental condition most often used is 37°C,
conducive to remaining far below saturation levels.
which corresponds to commonly accepted human core tem-
5.7.2 Sampling time points should also take into consider-
perature. Other temperatures may be appropriate for specific
ation the stability of the analyte. A theoretical decrease in
applications or clinical conditions.
biomolecule detection can be introduced due to the stability of
5.4.2 Temperature-controlled configurations described in
the released analyte, or changes to the analyte (see also 5.8.9.)
USP <711> and USP <724> may be appropriate and are
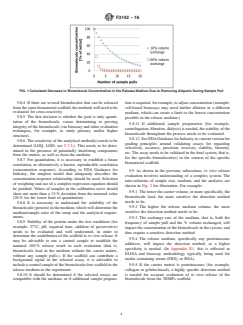
5.7.3 The frequency of sampling should be matched with
commercially available.Alternatively, appropriate vessels may
detectability in the assay (especially if the sample volume is
be placed in incubators or a water bath. Wrap-around tempera-
replaced after sampling, there is a constant dilution). Limit of
ture jackets may be appropriate for larger vessels.
quantitation (LOQ) and limit of detection (LOD) should be
5.4.3 Increasing the temperature to accelerate release may
understood. Fig. 1 illustrates the theoretical decrease in
or may not be appropriate, as the temperature may change the
biomolecule concentration in the release medium due to
characteristics or impact the integrity of the scaffold, and thus
removing aliquots during sample pull, using a 10 % and 66 %
alter the release mechanism (see Guide F2902). Temperature
sample volume exchange rate at each time point. At 66 %
also may impact the integrity of the biomolecule.
exchange, the initial total amount of the biomolecule in the
5.5 Static Conditions versus Dynamic Conditions:
system would be reduced to 10 % after only 2 time points.
5.5.1 The dissolution methods described in the USP are
5.7.4 Storage of release medium aliquots (condition and
adding a stirring movement or flow-through to facilitate
length of time before assaying) should be amenable to the
transport and distribution from the surface and immediate
biomolecule. Storage vials should be assessed for adsorption,
vicinity of the dosage form. A static system in vitro would
similar to the description in section 5.3.5.
likely also not be reflective of the in vivo situation for TEMPs,
5.8 Assay(s):
although it might be difficult to define a universal fluid flow
5.8.1 Careful consideration needs to be given to the selec-
simulating all anatomic sites and conditions.
tion of the analytical assay(s).
5.5.2 The physiologic condition at the most likely implan-
5.8.2 Literature review around characterization of parent-
tation scenario should be considered, for example, swelling
eraldrugdeliverysystemsandbiomaterialscaffoldscontaining
after surgery with considerable influx of fluid.
biomolecules revealed that the majority of in vitro release
5.5.3 Ph.Eur.2.9.25,dissolutiontestformedicatedchewing
experiments have been performed either with radioactively
gumsaddsamechanicalstresstosimulatethechewingmotion.
labeled compounds or by using immunosorbent-linked assays
Whilethestandardfrequency(describedas60perminute)may
for detection, or studying cell-based effects.
notbecompletelyappropriateforTEMPs,thegeneralprinciple
5.8.3 Thefirstapproachrequiresfacilitieswhereradioactive
andapparatusmightbeworthconsideringinthecasewherethe
material can be handled, and may not be feasible for final
implantation site, and thus the TEMPs construct, may be
product characterization for unitary products, as it requires
exposed to muscle movement.
labeling prior to combination with carrier materials. This in
5.6 Sampling Mechanism:
itself could possibly lead to changes in protein/carrier interac-
5.6.1 Options of pulling samples may be linked to or even
tion. Immunosorbent-linked assays may be difficult to realize
definedbythevesselandgeneralexperimentalsetup,aswellas
with high amounts of samples. For an industry laboratory, it
the assays conducted.
might be desirable to have an in vitro release assay where the
5.6.2 In general, the sample pulled may require some biomoleculecanbeanalyzedbystandardultraviolet(UV)light
separation of theTEMPs from the release medium.This can be spectroscopy or high performance liquid chromatography
achieved by sampling from the surface or a location remote (HPLC) methods and does not have to be labeled.
F3142 − 16
FIG. 1 Calculated Decrease in Biomolecule Concentration in the Release Medium Due to Removing Aliquots During Sample Pull
5.8.4 If there are several biomolecules that can be released tion is required, for example, to adjust concentration (example:
fromthesamebiomaterialscaffold,themethodswillneedtobe cell-based bioassays may need further dilution in a different
evaluated for cross-reactivity.
medium, which can create a limit to the lowest concentration
5.8.5 The first decision is whether the goal is only quanti-
possible in the release medium.)
tation of the biomolecule, versus determining or proving
5.8.11 If additional sample preparation (for example,
integrity of the biomolecule (via bioassay and other evaluation
centrifugation, filtration, dialysis) is needed, the stability of the
techniques, for example, to study primary and/or higher
biomolecule throughout the process needs to be evaluated.
structure).
5.8.12 SeeFDAGuidanceforIndustryorcurrentversionfor
5.8.6 The sensitivity of the analytical method(s) needs to be
guiding principles around validating assays for regarding
determined (LOQ, LOD; see 5.7.3.). This needs to be deter-
selectivity, accuracy, precision, recovery, stability, linearity,
mined in the presence of potentially interfering components
etc. The assay needs to be validated in the final system, that is,
from the matrix, as well as from the medium.
for the specific biomolecule(s) in the context of the specific
5.8.7 For quantitation, it is necessary to establish a linear
biomaterial scaffold.
correlation, or alternatively a known, reproducible correlation
(concentration response). According to FDA Guidance for
5.9 As shown in the previous subsections, in vitro release
Industry, the simplest model that adequately describes the
evaluation involves understanding of a complex system. The
concentration-response relationship should be used. Selection
inter-relations of sample size, medium, and the analytics are
of weighting and use of a complex regression equation should
shown in Fig. 2 for illustration. For example:
be justified. Values of samples in the calibration curve should
5.9.1 The lower the carrier volume, or more specifically, the
show not more than a 15 % deviation from the nominal value
biomolecule load, the more sensitive the detection method
(20 % for the lower limit of quantitation).
needs to be.
5.8.8 It is necessary to understand the solubility of the
5.9.2 The higher the release medium volume, the more
biomolecule (protein) in the medium, which will determine the
medium/sample ratio of the setup and the analytical require- sensitive the detection method needs to be.
ments.
5.9.3 The exchange rate of the medium, that is, both the
5.8.9 Stability of the protein under the test conditions (for
frequency of sample pull and the % volume exchanged, will
example, 37°C, pH, required time, addition of preservative)
impact the concentration of the biomolecule in the system, and
needs to be evaluated and well understood, in order to
thus require a sensitive detection method.
determine the contribution of the scaffold to in vitro release. It
5.9.4 The release medium, specifically any proteinaceous
may be advisable to run a control sample to establish the
additives, will impact the detection method, as a higher
nominal 100 % release result in each evaluation (that is,
specificity is needed. (In Appendix X1, this is reflected in
biomolecule load in the medium without the carrier matrix,
ELISA and bioassay methodology typically being used for
without any sample pulls.). If the scaffold can contribute a
media containing serum (FBS), or BSA).
background signal in the selected assay, it is advisable to
5.9.5 If the carrier matrix is proteinaceous (for example,
includeacontrolsampleofthebiomolecule-freescaffoldinthe
collagen or gelatin-based), a highly specific detection method
release medium in the experiment.
5.8.10 It should be determined if the selected assays are is needed for accurate evaluation of in vitro release of the
compatible with the medium, or if additional sample prepara- biomolecule from the TEMPs scaffold.
F3142 − 16
FIG. 2 Interrelationship of Factors in in vitro Release Experiments
APPENDIX
(Nonmandatory Information)
X1. PUBLISHED in-vitro RELEASE STUDIES PERFORMED WITH BIOMATERIAL SCAFFOLDS
LOADED WITH BIOMOLECULES
X1.1 Selection of studies on in vitro release from
biomolecule/biomaterial scaffold combinations (Table X1.1):
F3142 − 16
TABLE X1.1 Overview Table
(alphabetical order by biomolecule name)
Protein Carrier Release Medium and Setup Analytical Method Reference
bFGF Collagen films, heparinized 5 mL cell culture medium (5 % human serum) I, ELISA Wissink 2001 (4)
bFGF Collagen films Cell culture medium (5 % human serum) ELISA Wissink 2000 (5)
bFGF Gelatin PBS Fluorescence-labeled, HPLC Tabata 1998 (6)
bFGF; PLGA cylinders, microspheres; with Mg(OH) /BSA PBS + BSA + heparin Bradford protein assay; BIACORE (anti-BMP fixed) Zhu 2000 (7)
BMP-2
bFGF poly(ester urethane)urea scaffolds DNEM containing 0.5 % FBS and 1 % pen/strep I; rat vascular smooth muscle cell proliferation Guan 2007 (8)
rhbFGF chitosan-alginate scaffolds PBS ELISA; Hs68 cell proliferation Ho 2009 (9)
bFGF chitosan-hydroxyapatite scaffolds PBS with 0.1 % azide Fluorescence spectrophotometer (intrinsic Tigli 2009 (10)
tryptophan fluorescence)
BMP-2; Gelatin films (GTA-xl) Cell culture medium Bioassay (C3H10T1/2 — ALP activity; DNA Raiche 2001 (11)
BMP-4 content)
rhBMP-2 Collagen sponge, hyaluronic acid matrix, ceramics Bovine serum, 100 % exchange I D’Augusta 2000 (12)
rhBMP-2 PLGA microspheres PBS pH 7.4 (isotonic, or 0.1 M resp.) RP-HPLC Druggirala 1966a,b (13,
14)
rhBMP-2 Poly (D, L-lactide) disks Cell culture medium (5 % FBS) Bioassay (OPCI cells — ALP activity) Winn 1999 (15)
rhBMP-2 PLGA-hydroxyapatite scaffolds PBS ELISA; also used continuous Native-PAGE to Nie 2008 (16)
determine integrity and conformation of eluted
BMP-2
rhBMP-2 Dextran-derived microspheres PBS I; determined BMP activity using human Chen 2006 (17)
periodontal ligament cells (proliferation, ALP,
osteocalcin, and osteopontin)
rhBMP-2 PEG-PLGA microspheres PBS with 0.05 % polysorbate 20, 1 % BSA, 0.02 % ELISA; determined BMP activity using C2C12 Lochmann 2010 (18)
axide, and 0.15 % EDTA mouse myoblasts (ALP)
rhBMP-2 PLGA scaffolds DMEM containing 10 % FBS ELISA; determined BMP activity using rabbit MSCs Liu 2007 (19)
(proliferation, ALP, collagen, and mineralization)
rhMBP-2 PLGA microspheres in polyurenthane scaffolds Cell medium containing 1 % BSA ELISA; determined BMP activity using MC3T3 cells Li 2009 (20)
(ALP)
rhBMP-2 Hydroxyapatite-β-TCP DMEM containing 10 % FBS and 1 % pen/strep I Autefage 2009 (21)
Bovine calcitonin microparticles: PLGA, PET-PLGA PBS with polysorbate; tube versus dialysis bags I Diaz 1999 (22)
(sink)
BSA PLGA scaffold PBS (sink) Fluoraldehyde assay (Pierce) Whang 2000 (23)
BSA; PLGA PBS UV (280 nm); ELISA Eliaz 2000 (24)
sp55R
BSA, insulin Starch microspheres Phosphate buffer (pH=6.4) containing 3 mM azide, HPLC Elfstrand 2009
...



Questions, Comments and Discussion
Ask us and Technical Secretary will try to provide an answer. You can facilitate discussion about the standard in here.
Loading comments...