ASTM F3474-20
(Practice)Standard Practice for Establishing Exoskeleton Functional Ergonomic Parameters and Test Metrics
Standard Practice for Establishing Exoskeleton Functional Ergonomic Parameters and Test Metrics
SIGNIFICANCE AND USE
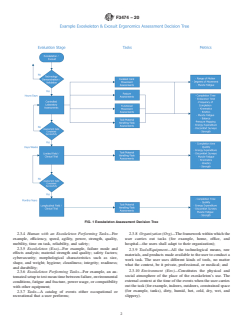
2.1 This practice describes what measure should be performed during the near (hours/days), mid (days/weeks), and far (months/years) stages of exoskeleton evaluation (Fig. 1). The functional conditions and metrics with respect to each task method are assessed from the body area(s) impacted by the exoskeleton (for example, upper body, lower body, or both). These may be within as well as distant to the body areas impacted by the exoskeleton (for example, an upper body exoskeleton may have impacts on the trunk and spine). Desired effects as well as unintended encumbrances to the user’s body are important considerations. The evaluation will occur within the context relevant to the end-use application of the exoskeleton’s implementation. This practice pertains to the industry, military, medical, first responders, and recreational domains, but other domains may arise in the future and will need to be considered. Each domain is unique unto itself; however, the task methods and metrics collected may be unique or overlap across any number of user domains.
FIG. 1 Exoskeleton Assessment Decision Tree
2.2 Task methods and their metrics are either administered in a laboratory environment, field environment, or both laboratory and field environments. Where not otherwise specified, patient functional outcome measures and pain are key metrics that should be considered for testing performed in the medical domain. Exoskeleton producers or researchers, or both, may also want to consider different types of imaging such as X-rays, computed tomography (CT) scans, magnetic resonance imaging (MRI), ultrasound, and nuclear medicine imaging. Additionally, exoskeleton producers or researchers, or both, may also wish to carry out neuroimaging such as, but not limited to, structural and functional and diffusion MRI, magnetoencephalography (MEG), electroencephalography (EEG), positron emission tomography (PET), or near infrared spectroscopy (NIRS) to understand the cognitive and neurophysiol...
SCOPE
1.1 This practice provides a recommended approach and a set of options for assessing one or more specific ergonomic parameters with respect to human users of exoskeletons.
1.2 This practice provides functional ergonomic criteria to consider for the design, production, and evaluation of exoskeletons within the domains of industry, military, medical, first responders, and recreational. When designing exoskeletons, natural unassisted human kinematics and kinetics, as well as the resulting strain and fatigue experienced by the user should be salient design parameters. Any changes in the natural unassisted human kinematics and kinetics may impact the exoskeleton’s effectiveness in augmenting user performance. Therefore, the defining principle of this practice is to establish objective measures that can be selected from to assess human kinematics and kinetics, as well as the resulting strain and fatigue experienced by the user within the task context of the exoskeleton’s end use application.
1.3 This standard does not purport to address all of the safety concerns, if any, associated with its use. It is the responsibility of the user of this standard to establish appropriate safety, health, and environmental practices and determine the applicability of regulatory limitations prior to use.
1.4 This international standard was developed in accordance with internationally recognized principles on standardization established in the Decision on Principles for the Development of International Standards, Guides and Recommendations issued by the World Trade Organization Technical Barriers to Trade (TBT) Committee.
General Information
- Status
- Published
- Publication Date
- 14-Dec-2020
- Technical Committee
- F48 - Exoskeletons and Exosuits
- Drafting Committee
- F48.02 - Human Factors and Ergonomics
Overview
ASTM F3474-20 is the international standard practice developed by ASTM International for establishing functional ergonomic parameters and test metrics of exoskeletons. This standard outlines a comprehensive and structured methodology for assessing the ergonomic impact of exoskeletons across various application domains, including industry, military, medical, first responders, and recreational activities. It provides a recommended approach and options for evaluating both intended improvements and any potential encumbrances to the user, considering both short- and long-term usage.
Key Topics
- Ergonomic Evaluation Stages: The standard describes assessment stages for exoskeletons, covering near (hours/days), mid (days/weeks), and far (months/years) periods. This ensures a consistent approach to evaluating effectiveness and user impact over time.
- Task Methods and Metrics: Specifies laboratory and field test methods for assessing tasks relevant to upper body, lower body, or combined exoskeletons. Metrics include objective and subjective measures such as range of motion, muscle activation, metabolic cost, pain ratings, and task completion.
- Domain-Specific Considerations: Provides functional ergonomic criteria pertinent to the exoskeleton’s use context, including industry, military, medical, first responders, and recreational settings. For example, in the medical domain, patient functional outcomes and pain metrics are key.
- Body Area Impacts: Addresses both localized (e.g., upper or lower body) and distant effects (e.g., upper limb exoskeleton affecting the spine or trunk), ensuring holistic user assessment.
- Objective and Subjective Measures: Encourages the use of both quantitative measures (e.g., joint angles, strength, physiological signals) and qualitative assessments (e.g., comfort, perceived exertion).
- Imaging and Neuroimaging: Recommends considering advanced techniques such as X-ray, MRI, CT, MEG, EEG, PET, and NIRS for a comprehensive understanding of the exoskeleton’s physiological and neurophysiological impacts.
Applications
ASTM F3474-20 supports a wide range of practical applications in the development, production, and evaluation of exoskeletons:
- Industrial Exoskeletons: Enhancing worker safety, reducing fatigue and strain, and improving productivity through ergonomic task analysis and validation.
- Medical Exoskeletons: Supporting rehabilitation and mobility by using functional outcome and pain measures to track patient progress and optimize device fit.
- Military and First Responders: Improving performance in dynamic, physically demanding tasks with metrics tailored for evaluating mobility, agility, and task reliability under real-world conditions.
- Recreational Use: Assessing ergonomic support for activities such as hiking or sports, where comfort and movement efficiency are paramount.
- Research and Development: Informing exoskeleton design through standardized metrics, ensuring user safety, long-term effectiveness, and regulatory compliance.
Related Standards
- ASTM F3323: Standard guide for labeling exoskeletons and exosuits, providing complementary guidance for clear product information and safe use.
- ASTM F3517: Standard practice for system safety of exoskeletons, focusing on the broader safety framework for exoskeleton deployment.
- ISO 13482: International standard for the safety requirements of personal care robots, often referenced for exoskeletons.
- Other Ergonomics and Biomechanics Standards: Related testing protocols for human factors and ergonomic assessment.
In summary, ASTM F3474-20 sets the foundational framework for evaluating the ergonomic parameters and test metrics essential for the safe and effective integration of exoskeletons into diverse domains. Its practical approach enables designers, manufacturers, and end users to optimize performance, mitigate risks, and realize the full potential of exoskeleton technology. For organizations involved in the development or deployment of exoskeletons, adoption of this standard ensures alignment with best practices and international expectations for ergonomic performance and user well-being.
Buy Documents
ASTM F3474-20 - Standard Practice for Establishing Exoskeleton Functional Ergonomic Parameters and Test Metrics
Get Certified
Connect with accredited certification bodies for this standard

BSI Group
BSI (British Standards Institution) is the business standards company that helps organizations make excellence a habit.

TÜV Rheinland
TÜV Rheinland is a leading international provider of technical services.

TÜV SÜD
TÜV SÜD is a trusted partner of choice for safety, security and sustainability solutions.
Sponsored listings
Frequently Asked Questions
ASTM F3474-20 is a standard published by ASTM International. Its full title is "Standard Practice for Establishing Exoskeleton Functional Ergonomic Parameters and Test Metrics". This standard covers: SIGNIFICANCE AND USE 2.1 This practice describes what measure should be performed during the near (hours/days), mid (days/weeks), and far (months/years) stages of exoskeleton evaluation (Fig. 1). The functional conditions and metrics with respect to each task method are assessed from the body area(s) impacted by the exoskeleton (for example, upper body, lower body, or both). These may be within as well as distant to the body areas impacted by the exoskeleton (for example, an upper body exoskeleton may have impacts on the trunk and spine). Desired effects as well as unintended encumbrances to the user’s body are important considerations. The evaluation will occur within the context relevant to the end-use application of the exoskeleton’s implementation. This practice pertains to the industry, military, medical, first responders, and recreational domains, but other domains may arise in the future and will need to be considered. Each domain is unique unto itself; however, the task methods and metrics collected may be unique or overlap across any number of user domains. FIG. 1 Exoskeleton Assessment Decision Tree 2.2 Task methods and their metrics are either administered in a laboratory environment, field environment, or both laboratory and field environments. Where not otherwise specified, patient functional outcome measures and pain are key metrics that should be considered for testing performed in the medical domain. Exoskeleton producers or researchers, or both, may also want to consider different types of imaging such as X-rays, computed tomography (CT) scans, magnetic resonance imaging (MRI), ultrasound, and nuclear medicine imaging. Additionally, exoskeleton producers or researchers, or both, may also wish to carry out neuroimaging such as, but not limited to, structural and functional and diffusion MRI, magnetoencephalography (MEG), electroencephalography (EEG), positron emission tomography (PET), or near infrared spectroscopy (NIRS) to understand the cognitive and neurophysiol... SCOPE 1.1 This practice provides a recommended approach and a set of options for assessing one or more specific ergonomic parameters with respect to human users of exoskeletons. 1.2 This practice provides functional ergonomic criteria to consider for the design, production, and evaluation of exoskeletons within the domains of industry, military, medical, first responders, and recreational. When designing exoskeletons, natural unassisted human kinematics and kinetics, as well as the resulting strain and fatigue experienced by the user should be salient design parameters. Any changes in the natural unassisted human kinematics and kinetics may impact the exoskeleton’s effectiveness in augmenting user performance. Therefore, the defining principle of this practice is to establish objective measures that can be selected from to assess human kinematics and kinetics, as well as the resulting strain and fatigue experienced by the user within the task context of the exoskeleton’s end use application. 1.3 This standard does not purport to address all of the safety concerns, if any, associated with its use. It is the responsibility of the user of this standard to establish appropriate safety, health, and environmental practices and determine the applicability of regulatory limitations prior to use. 1.4 This international standard was developed in accordance with internationally recognized principles on standardization established in the Decision on Principles for the Development of International Standards, Guides and Recommendations issued by the World Trade Organization Technical Barriers to Trade (TBT) Committee.
SIGNIFICANCE AND USE 2.1 This practice describes what measure should be performed during the near (hours/days), mid (days/weeks), and far (months/years) stages of exoskeleton evaluation (Fig. 1). The functional conditions and metrics with respect to each task method are assessed from the body area(s) impacted by the exoskeleton (for example, upper body, lower body, or both). These may be within as well as distant to the body areas impacted by the exoskeleton (for example, an upper body exoskeleton may have impacts on the trunk and spine). Desired effects as well as unintended encumbrances to the user’s body are important considerations. The evaluation will occur within the context relevant to the end-use application of the exoskeleton’s implementation. This practice pertains to the industry, military, medical, first responders, and recreational domains, but other domains may arise in the future and will need to be considered. Each domain is unique unto itself; however, the task methods and metrics collected may be unique or overlap across any number of user domains. FIG. 1 Exoskeleton Assessment Decision Tree 2.2 Task methods and their metrics are either administered in a laboratory environment, field environment, or both laboratory and field environments. Where not otherwise specified, patient functional outcome measures and pain are key metrics that should be considered for testing performed in the medical domain. Exoskeleton producers or researchers, or both, may also want to consider different types of imaging such as X-rays, computed tomography (CT) scans, magnetic resonance imaging (MRI), ultrasound, and nuclear medicine imaging. Additionally, exoskeleton producers or researchers, or both, may also wish to carry out neuroimaging such as, but not limited to, structural and functional and diffusion MRI, magnetoencephalography (MEG), electroencephalography (EEG), positron emission tomography (PET), or near infrared spectroscopy (NIRS) to understand the cognitive and neurophysiol... SCOPE 1.1 This practice provides a recommended approach and a set of options for assessing one or more specific ergonomic parameters with respect to human users of exoskeletons. 1.2 This practice provides functional ergonomic criteria to consider for the design, production, and evaluation of exoskeletons within the domains of industry, military, medical, first responders, and recreational. When designing exoskeletons, natural unassisted human kinematics and kinetics, as well as the resulting strain and fatigue experienced by the user should be salient design parameters. Any changes in the natural unassisted human kinematics and kinetics may impact the exoskeleton’s effectiveness in augmenting user performance. Therefore, the defining principle of this practice is to establish objective measures that can be selected from to assess human kinematics and kinetics, as well as the resulting strain and fatigue experienced by the user within the task context of the exoskeleton’s end use application. 1.3 This standard does not purport to address all of the safety concerns, if any, associated with its use. It is the responsibility of the user of this standard to establish appropriate safety, health, and environmental practices and determine the applicability of regulatory limitations prior to use. 1.4 This international standard was developed in accordance with internationally recognized principles on standardization established in the Decision on Principles for the Development of International Standards, Guides and Recommendations issued by the World Trade Organization Technical Barriers to Trade (TBT) Committee.
ASTM F3474-20 is classified under the following ICS (International Classification for Standards) categories: 11.180.10 - Aids and adaptation for moving; 25.040.30 - Industrial robots. Manipulators. The ICS classification helps identify the subject area and facilitates finding related standards.
ASTM F3474-20 is available in PDF format for immediate download after purchase. The document can be added to your cart and obtained through the secure checkout process. Digital delivery ensures instant access to the complete standard document.
Standards Content (Sample)
This international standard was developed in accordance with internationally recognized principles on standardization established in the Decision on Principles for the
Development of International Standards, Guides and Recommendations issued by the World Trade Organization Technical Barriers to Trade (TBT) Committee.
Designation: F3474 − 20
Standard Practice for
Establishing Exoskeleton Functional Ergonomic Parameters
and Test Metrics
This standard is issued under the fixed designation F3474; the number immediately following the designation indicates the year of
original adoption or, in the case of revision, the year of last revision. A number in parentheses indicates the year of last reapproval. A
superscript epsilon (´) indicates an editorial change since the last revision or reapproval.
1. Scope exoskeleton (for example, upper body, lower body, or both).
These may be within as well as distant to the body areas
1.1 This practice provides a recommended approach and a
impacted by the exoskeleton (for example, an upper body
set of options for assessing one or more specific ergonomic
exoskeletonmayhaveimpactsonthetrunkandspine).Desired
parameters with respect to human users of exoskeletons.
effects as well as unintended encumbrances to the user’s body
1.2 This practice provides functional ergonomic criteria to
are important considerations. The evaluation will occur within
consider for the design, production, and evaluation of exoskel-
the context relevant to the end-use application of the exoskel-
etons within the domains of industry, military, medical, first
eton’s implementation. This practice pertains to the industry,
responders, and recreational. When designing exoskeletons,
military, medical, first responders, and recreational domains,
natural unassisted human kinematics and kinetics, as well as
but other domains may arise in the future and will need to be
the resulting strain and fatigue experienced by the user should
considered. Each domain is unique unto itself; however, the
be salient design parameters. Any changes in the natural
task methods and metrics collected may be unique or overlap
unassisted human kinematics and kinetics may impact the
across any number of user domains.
exoskeleton’s effectiveness in augmenting user performance.
Therefore, the defining principle of this practice is to establish
2.2 Task methods and their metrics are either administered
objective measures that can be selected from to assess human
in a laboratory environment, field environment, or both labo-
kinematics and kinetics, as well as the resulting strain and
ratory and field environments. Where not otherwise specified,
fatigue experienced by the user within the task context of the
patient functional outcome measures and pain are key metrics
exoskeleton’s end use application.
that should be considered for testing performed in the medical
1.3 This standard does not purport to address all of the
domain. Exoskeleton producers or researchers, or both, may
safety concerns, if any, associated with its use. It is the
alsowanttoconsiderdifferenttypesofimagingsuchasX-rays,
responsibility of the user of this standard to establish appro-
computed tomography (CT) scans, magnetic resonance imag-
priate safety, health, and environmental practices and deter-
ing (MRI), ultrasound, and nuclear medicine imaging.
mine the applicability of regulatory limitations prior to use.
Additionally, exoskeleton producers or researchers, or both,
1.4 This international standard was developed in accor-
may also wish to carry out neuroimaging such as, but not
dance with internationally recognized principles on standard-
limited to, structural and functional and diffusion MRI, mag-
ization established in the Decision on Principles for the
netoencephalography (MEG), electroencephalography (EEG),
Development of International Standards, Guides and Recom-
positron emission tomography (PET), or near infrared spec-
mendations issued by the World Trade Organization Technical
troscopy (NIRS) to understand the cognitive and neurophysi-
Barriers to Trade (TBT) Committee.
ological impacts that exoskeletons have on the brain.
2. Significance and Use
2.3 Fig. 2 is a Venn diagram that portrays the distinct
2.1 This practice describes what measure should be per- interactions that may transpire between the user (human),
formedduringthenear(hours/days),mid(days/weeks),andfar exoskeleton, and task. The interactions are:
(months/years) stages of exoskeleton evaluation (Fig. 1). The
2.3.1 Human—For example, baseline health, physiology,
functional conditions and metrics with respect to each task
and job duty assessment;
method are assessed from the body area(s) impacted by the
2.3.2 Human with an Exoskeleton—For example, fit,
comfort, physical size changes, psychosocial considerations,
cognitive load, training level, donning/doffing time, and safety;
This practice is under the jurisdiction of ASTM Committee F48 on Exoskel-
etons and Exosuits and is the direct responsibility of Subcommittee F48.02 on
2.3.3 Human Performing Tasks—For example, efficiency,
Human Factors and Ergonomics.
speed, agility, power, strength, quality, mobility, time on task,
Current edition approved Dec. 15, 2020. Published January 2021. DOI: 10.1520/
F3474-20. and safety;
Copyright © ASTM International, 100 Barr Harbor Drive, PO Box C700, West Conshohocken, PA 19428-2959. United States
F3474 − 20
FIG. 1 Exoskeleton Assessment Decision Tree
2.3.4 Human with an Exoskeleton Performing Tasks—For 2.3.8 Organization (Org)—Theframeworkwithinwhichthe
example, efficiency, speed, agility, power, strength, quality, user carries out tasks (for example, home, office, and
mobility, time on task, reliability, and safety;
hospital—the users shall adapt to their organization);
2.3.5 Exoskeleton (Exo)—For example, failure mode and
2.3.9 Tools/Equipment—All the technological means, raw
effects analysis; material strength and quality; safety factors;
materials, and products made available to the user to conduct a
cybersecurity; morphological characteristics such as size,
work task. The user uses different kinds of tools, no matter
shape, and weight; hygiene; cleanliness; integrity; readiness;
what the context, be it private, professional, or medical; and
and durability;
2.3.10 Environment (Env)—Constitutes the physical and
2.3.6 Exoskeleton Performing Tasks—For example, an au-
social atmosphere of the place of the exoskeleton’s use. The
tomatedsetuptotestmeantimebetweenfailure,environmental
external context at the time of the events when the user carries
conditions, fatigue and fracture, power usage, or compatibility
out the task (for example, indoors, outdoors, constrained space
with other equipment;
(for example, tanks), dirty, humid, hot, cold, dry, wet, and
2.3.7 Tasks—A catalog of events either occupational or
slippery).
recreational that a user performs;
F3474 − 20
FIG. 2 Exoskeleton Performance Interaction Diagram
2.4 This methodology indicates considerations that exoskeleton. The decision tree is modulated temporally in
employers/users should use to govern which jobs are more
which assessments occur at hours/days, days/weeks, and
suited to just humans versus humans with exoskeletons. Based
months/years. This decision tree complements the task meth-
on those results, human exoskeleton assessments can be
ods in Section 4 with respect to when an assessment should be
performed using the ergonomic assessment decision chart to
conducted.
determine exoskeleton efficacy with respect to the task(s).
From there, the human, exoskeleton, and task(s) are integrated
4. Ergonomic Task Methods
into the organization (where applicable based on domain),
4.1 Isolated Joint Movement:
tools/equipment, and environment of utilization. Furthermore,
when conducting an assessment, please see Practice for Docu-
4.1.1 Passive Joint Range of Motion—Passive joint range of
menting Environmental Conditions for Utilization with Exo- motioncanbeapplicablethroughoutthebody.Passiverangeof
skeleton Test Methods for environmental ramifications.
motion is the arc of motion produced by the application of an
external force by an examiner, gravity, or external source.
2.5 Depending on the context in which the exoskeleton is
These changes reflect angular displacements unique to the
used (medical, industrial, military, first responders, and
respective joint. Assessments of passive joint range of motion
recreational), it is necessary to take into account these comple-
can be conducted in a laboratory or field environment associ-
mentary characteristics to integrate the exoskeletons better.
ated with the industrial, military, medical, first responders, and
3. Ergonomic Assessment Decision Chart
recreationaldomains.Suchmeasuresaredegreesofmovement,
3.1 Fig. 1 is a decision tree that categorizes the evaluation
range of motion, and strength assessments. Subjective mea-
stages, tasks, and metrics for the objective assessment of an
sures as the user performs the task are psychophysical and
psychophysiological metrics (rating of pain, soreness,
Unpublished ASTM standard in development. discomfort, or comfort, or combinations thereof).
F3474 − 20
4.1.2 Active Joint Range of Motion—These changes reflect postural sway, pressure mapping, and completion time. Sub-
angular displacements unique to the respective joint. Active jectivemeasuresastheuserperformsthetaskarepsychophysi-
range of motion is the arc of motion produced by an individu- cal and psychophysiological metrics (RPE, rating of pain,
al’s voluntary unassisted muscle contraction, joint mobility, soreness, discomfort, or comfort, or combinations thereof). A
andtheresultantmovementofpart(s)ofthebody.Assessments
measure to account for incidents of falls or loss of balance is
ofactivejointrangeofmotioncanbeconductedinalaboratory important for industrial, military, medical, first responders, and
or field environment associated with industrial, military,
recreational domains.
medical, first responders, and recreational domains. Objective
4.2.2 Seated Task—Seated task covers a chair, bench, or
measures are electromyography, degrees of movement, range
stool without a back; chair, bench, or stool with a back; and
of motion, and strength assessments. Subjective measures as
using the ground as a seating surface.Assessments of a seated
the user performs the task are psychophysical and psycho-
task can be conducted in a laboratory or field environment
physiological metrics (rate of perceived exertion (RPE), rating
associated with industrial, military, medical, first responders,
of pain, soreness, discomfort, or comfort, or combinations
and recreational domains. Seated tasks encompass the entire
thereof).
body.
4.1.3 Workspace or Reach Envelope—Workspace or reach
4.2.2.1 Seated With or Without a Chair Back—Seated with
envelope affords two- and three-dimensional (2 and 3D) joint
or without a chair back objective measures are blood pressure,
or limb range of motion (for example, movement through one
blood-oxygen saturation, durations of maintaining the posture,
or multiple planes) of the upper and lower body extremities.
ability to obtain the posture, seated stability (center of
Assessmentsofaworkspaceorreachvolumecanbeconducted
pressure), muscle activation/fatigue (EMG, integrated muscle
in a laboratory or field environment associated with industrial,
activity, time of muscle activity onset, frequency component
military, medical, first responders, and recreational domains.
analysis, muscle synergies, or co-contraction, or combinations
The envelope is quantified by a workspace volume, which is
thereof), metabolic/energy cost (rate of oxygen consumption,
measured quantitatively in cubic measurements.
kilocalories expended, cost of transport, heart rate, heart rate
4.2 Posture and Movement: variability, respiratory exchange ratio, and VO max), NIRS,
functional completion, joint/spine stresses (biomechanics), bi-
4.2.1 Standing Balance Assessment—Standing balance as-
nary fit changes, skin interface (shear, pressure, friction, and
sessment is bifurcated between static and dynamic analyses.
thermal), postural sway, and 3D changes of body segments and
This assessment is applicable to the entire body. Assessments
limbs. Subjective measures as the user performs the task are
of standing balance assessment can be conducted in a labora-
psychophysical and psychophysiological metrics (RPE, rating
tory or field environment associated with the industrial,
of pain, soreness, discomfort, or comfort, or combinations
military, medical, first responders, and recreational domains.
thereof).
4.2.1.1 Static Standing Balance—Static standing balance
4.2.2.2 Seated on the Ground—Seated on the ground objec-
can either be symmetrical, staggered, split, tandem, or single-
tive measures are blood pressure, blood-oxygen saturation,
leg stance. Objective measures are center of pressure muscle
activation/fatigue (electromyography (EMG), integrated durations of maintaining the posture, ability to obtain the
posture, seated stability (center of pressure), muscle activation/
muscle activity, time of muscle activity onset, frequency
component analysis, muscle synergies, or co-contraction, or fatigue (EMG, integrated muscle activity, time of muscle
activity onset, frequency component analysis, muscle
combinations thereof), metabolic/energy cost (rate of oxygen
consumption, kilocalories expended, cost of transport, heart synergies, or co-contraction, or combinations thereof),
metabolic/energy cost (rate of oxygen consumption, kilocalo-
rate, heart rate variability, respiratory exchange ratio, and
maximal oxygen uptake (VO ) max), blood pressure, blood- ries expended, cost of transport, heart rate, heart rate
variability, respiratory exchange ratio, and VO max), NIRS,
oxygen saturation, near infrared spectroscopy, motion capture,
postural sway, center of gravity, and pressure mapping. Sub- functional completion, joint/spine stresses (biomechanics), bi-
nary fit changes, skin interface (shear, pressure, friction, and
jectivemeasuresastheuserperformsthetaskarepsychophysi-
thermal), postural sway, and 3D changes of body segments and
cal and psychophysiological metrics (RPE, rating of pain,
limbs. Subjective measures as the user performs the task are
soreness, discomfort, or comfort, or combinations thereof).
psychophysical and psychophysiological metrics (RPE, rating
4.2.1.2 Dynamic Standing Balance—Dynamic standing bal-
of pain, soreness, discomfort, or comfort, or combinations
ance can be assessed using equipment such as balance boards,
thereof).
balance beams, and incline/decline slopes. It can be assessed in
symmetrical, staggered, split, tandem, or single-leg stance. 4.2.3 Awkward Postures—Awkward postures can be de-
Objective measures are blood pressure, blood-oxygen scribed as non-neutral postures. Non-neutral postures place the
saturation, center of pressure, muscle activation/fatigue (EMG, user’s body in positions of misalignment. Upper body areas
integrated muscle activity, time of muscle activity onset, specific to misalignment are the neck, shoulder, elbow,
frequency component analysis, muscle synergies, or co- forearm, wrist, and hand. Awkward postures can also apply to
contraction, or combinations thereof), metabolic/energy cost the trunk/torso, spine, pelvis, hips, knees, ankles, and feet.
(rate of oxygen consumption, kilocalories expended, cost of These misalignments can increase strain on the surrounding
transport, heart rate, heart rate variability, respiratory exchange tissues and can cause uneven wear and eventual potential
ratio, and VO max), blood pressure, blood-oxygen saturation, damage to soft tissues and joints. When awkward postures are
near infrared spectroscopy, motion capture, center of gravity, sustainedoverextendeddurations,reducedbloodflowtotissue
F3474 − 20
often results, which can exacerbate suboptimal conditions for ery (returning back to neutral posture). Subjective measures as
the user at a greater rate.Wear of an exoskeleton may increase, the user performs the task are psychophysical and psycho-
decrease, or affect in a different manner the frequency and physiological metrics (RPE, rating of pain, soreness,
duration of the awkward posture. Assessments of awkward
discomfort, or comfort, or combinations thereof). Lastly, all
postures can be performed in both laboratory and field envi-
domains should be concerned with quality of movement.
ronments associated with industrial, military, medical, first
4.2.3.3 Torso—The torso encompasses the entire body. This
responders, and recreational domains. Objective measures are
task’s context is flexion (anterior movement), extension (pos-
duration of maintaining the posture, the ability to obtain the
terior movement), rotation, and side bending (lateral move-
posture, blood pressure, blood-oxygen saturation, muscle
ment) at the trunk where the feet are planted and the lower
activation/fatigue (EMG, integrated muscle activity, time of
body is mostly static. Torso assessments can be conducted in a
muscle activity onset, frequency component analysis, muscle
laboratory or field environment associated with industrial,
synergies, or co-contraction, or combinations thereof),
military, medical (patient centric), first responder, and recre-
metabolic/energy cost (rate of oxygen consumption, kilocalo-
ational domains. Objective measures are range of motion,
ries expended, cost of transport, heart rate, heart rate
binary task completion, muscle activation/fatigue (EMG, inte-
variability, respiratory exchange ratio, and VO max), NIRS,
gratedmuscleactivity,timeofmuscleactivityonset,frequency
functional completion/effectivity tasks, joint/spinal stresses
component analysis, muscle synergies, or co-contraction, or
(biomechanics), binary fit changes, skin interface (shear,
combinations thereof), metabolic/energy cost (rate of oxygen
pressure, friction, and thermal), 3D volumetric changes of
consumption, kilocalories expended, cost of transport, heart
bodysegments/limbs,andpressurepoints.Subjectivemeasures
rate, heart rate variability, respiratory exchange ratio, and VO
as the user performs the task are psychophysical and psycho-
max), NIRS, joint/spinal stresses (biomechanics), skin inter-
physiological metrics (RPE, rating of pain, soreness,
discomfort, or comfort, or combinations thereof). All domains face (shear, pressure, friction, and thermal), functional
leverage functional completion/effectivity, and military and completion/effectivitytasks,duration/frequencyofmaintaining
law enforcement should consider weapons and armor. the posture, postural stability, and postural recovery (returning
back to neutral posture). Subjective measures as the user
4.2.3.1 Lying Prone or Supine—Lying prone or supine
performs the task are psychophysical and psychophysiological
affects the entire body segments of exoskeleton users. Assess-
ments of lying prone or supine can be conducted in laboratory metrics (RPE, rating of pain, soreness, discomfort, or comfort,
or field environments associated with industrial, military, or combinations thereof). Additionally, for all domains, func-
medical, first responder, and recreational domains. Objective
tional completion/effectivity are significant, and military and
measures are heart rate, heart rate variability, blood pressure,
law enforcement should consider weapons and armor. Lastly,
blood-oxygen saturation, duration of maintaining the posture,
the medical domain is concerned with quality of movement,
ability to obtain the posture, heart rate variability, functional
functional outcome measures, and pain capture.
completion/effectivity tasks, joint/spinal stresses
4.2.4 Kneel—A kneel, either with single or double knee
(biomechanics), binary fit changes, skin interface (shear,
involves the trunk/torso and lower body. Tasks may be per-
pressure, friction, and thermal), 3D volumetric changes of
formed in kneeling that also involve the upper body. Assess-
bodysegments/limbs,andpressurepoints.Subjectivemeasures
ments of a kneel can be conducted in a laboratory or field
as the user performs the task are psychophysical and psycho-
environment associated with industrial, military, medical, first
physiological metrics (RPE, rating of pain, soreness,
responder, and recreational domains. Objective measures are
discomfort, or comfort, or combinations thereof). All domains
blood pressure, blood-oxygen saturation, muscle activation/
may include functional completion/effectivity and completion
fatigue (EMG, integrated muscle activity, time of muscle
times, and military and law enforcement should consider
activity onset, frequency component analysis, muscle
weapons and armor.
synergies, or co-contraction, or combinations thereof),
4.2.3.2 Neck—The neck encompasses only head movement.
metabolic/energy cost (rate of oxygen consumption, kilocalo-
This task’s context is flexion (anterior movement), extension
ries expended, cost of transport, heart rate, heart rate
(posterior movement), side bending (lateral movement), and
variability, respiratory exchange ratio, and VO max), NIRS,
rotation at the cervical vertebrae where the torso is static or
duration of maintaining the posture, ability to obtain the
representative of the task under evaluation. Neck assessments
posture, kneeling stability (center of pressure), heart rate
can be conducted in a laboratory or field environment associ-
variability, functional completion/effectivity tasks, joint/spinal
ated with industrial, military, medical (patient centric), first
stresses (biomechanics), binary fit changes, skin interface
responder, and recreational domains. Objective measures are
(shear, pressure, friction, and thermal), postural sway, and 3D
relative movement between helmet and head, range of motion,
volumetric changes of body segments/limbs. Subjective mea-
binary task completion, muscle activation/fatigue (EMG, inte-
sures as the user performs the task are psychophysical and
gratedmuscleactivity,timeofmuscleactivityonset,frequency
psychophysiological metrics (RPE, rating of pain, soreness,
component analysis, muscle synergies, or co-contraction, or
discomfort, or comfort, or combinations thereof).Additionally,
combinations thereof), joint/spinal stresses (biomechanics),
for all domains, functional completion/effectivity and comple-
skin interface (shear, pressure, friction, and thermal), func-
tion times are of significance, and military and law enforce-
tional completion/effectivity tasks, duration/frequency of
maintaining the posture, postural stability, and postural recov- ment should consider weapons and armor.
F3474 − 20
4.2.5 Shoulder Mobility—Shoulder mobility mainly encom- 4.2.6 Squat—A squat encompasses the entire body. Assess-
passes the upper body and the trunk/torso. The shoulder is a ments of a squat can be conducted in a laboratory or field
very mobile joint. When shoulder mobility is tested while the environment associated with industrial, military, medical, first
user performs a task involving the lower body, the lower body responder, and recreational domains. Objective measures are
may also be of interest. This task’s context is moving forward range of motion, binary task completion, 3D volumetric
(flexion), backwards (extension), sideways (abduction and changes of body segments/limbs, muscle activation/fatigue
(EMG, integrated muscle activity, time of muscle activity
adduction), and rotating (internally and externally) at the
shoulder. Internal and external rotation can be completed with onset, frequency component analysis, muscle synergies, or
the shoulder maintained in any range of motion. Finally, the co-contraction, or combinations thereof), metabolic/energy
evaluation can integrate horizontal abduction, horizontal cost (rate of oxygen consumption, kilocalories expended, cost
adduction, or circumduction.Assessments of shoulder mobility of transport, heart rate, heart rate variability, respiratory ex-
change ratio, and VO max), NIRS, joint/spinal stresses
can be conducted in a laboratory or field environment associ-
(biomechanics), skin interface (shear, pressure, friction, and
ated with industrial, military, medical, first responder, and
thermal), functional completion/effectivity tasks, and duration/
recreational domains. Objective measures are range of motion,
frequency of maintaining the posture. Subjective measures as
binary task completion, 3D volumetric changes of body
the user performs the task are psychophysical and psycho-
segments/limbs, muscle activation/fatigue (EMG, integrated
physiological metrics (RPE, rating of pain, soreness,
muscle activity, time of muscle activity onset, frequency
discomfort, or comfort, or combinations thereof).Additionally,
component analysis, muscle synergies, or co-contraction, or
for all domains, functional completion/effectivity and comple-
combinations thereof), metabolic/energy cost (rate of oxygen
tion times are significant and should be considered, and
consumption, kilocalories expended, cost of transport, heart
military and law enforcement should consider weapons and
rate, heart rate variability, respiratory exchange ratio, and VO
armor.
max), NIRS, joint/spinal stresses (biomechanics), skin inter-
face (shear, pressure, friction, and thermal), functional 4.2.7 Stoop or Bend—Stoop or bend involves the entire
completion/effectivity tasks, and duration/frequency of main-
body. The legs during this task are fairly straight and the
taining the posture, postural stability, and postural recovery trunk/torso and upper body are bending at the waist. Assess-
(returning back to neutral posture). Subjective measures as the ments of a stoop or bend can be conducted in a laboratory or
user performs the task are psychophysical and psychophysi- field environment associated with industrial, military, medical,
ological metrics (RPE, rating of pain, soreness, discomfort, or first responder, and recreational domains. Objective measures
comfort, or combinations thereof). are range of motion, binary task completion, 3D volumetric
changes of body segments/limbs, muscle activation/fatigue
4.2.5.1 Arms at or Above Shoulder—The arms above shoul-
(EMG, integrated muscle activity, time of muscle activity
ders movement mostly applies to the upper body and trunk/
onset, frequency component analysis, muscle synergies, or
torso, although tasks may be performed involving this posture
co-contraction, or combinations thereof), metabolic/energy
in standing which also involved the lower body. This task area
cost (rate of oxygen consumption, kilocalories expended, cost
delineates overhead work, hands or arms would be above
of transport, heart rate, heart rate variability, respiratory ex-
shoulders and the torso would be upright.Assessments of arms
change ratio, and VO max), NIRS, joint/spinal stresses
above shoulders can be conducted in a laboratory or field 2
(biomechanics), skin interface (shear, pressure, friction, and
environment associated with industrial, military, medical, first
thermal), functional completion/effectivity tasks, completion
responders, and recreational domains. Objective measures are
times, and duration/frequency of maintaining the posture.
range of motion, binary task completion, 3D volumetric
Subjective measures as the user performs the task are psycho-
changes of body segments/limbs, muscle activation/fatigue
physical and psychophysiological metrics (RPE, rating of pain,
(EMG, integrated muscle activity, time of muscle activity
soreness, discomfort, or comfort, or combinations thereof).
onset, frequency component analysis, muscle synergies, or
Additionally, military and law enforcement should consider
co-contraction, or combinations thereof), blood pressure,
weapons and armor.
blood-oxygen saturation, metabolic/energy cost (rate of oxy-
gen consumption, kilocalories expended, cost of transport, 4.2.8 Forward Lunge—Forward lunge involves the entire
heart rate, heart rate variability, respiratory exchange ratio, and body. The foot position is one foot in front of the other at a set
VO max), NIRS, joint/spinal stresses (biomechanics), skin length (staggered or split stance). Assessments of a forward
interface (shear, pressure, friction, and thermal), functional lunge can be conducted in a laboratory or field environment
completion/effectivity/accuracy/precision tasks, duration/ associated with industrial, military, medical, first responder,
frequency of maintaining the posture, and strength assessment. and recreational domains. Objective measures are range of
Subjective measures as the user performs the task are psycho- motion, binary task completion, 3D volumetric changes of
physical and psychophysiological metrics (RPE, rating of pain, body segments/limbs, muscle activation/fatigue (EMG, inte-
soreness, discomfort, or comfort, or combinations thereof). gratedmuscleactivity,timeofmuscleactivityonset,frequency
Additionally, for all domains functional completion/effectivity component analysis, muscle synergies, or co-contraction, or
and completion times are significant and should be considered, combinations thereof), metabolic/energy cost (rate of oxygen
and military and law enforcement should consider weapons consumption, kilocalories expended, cost of transport, heart
and armor. rate, heart rate variability, respiratory exchange ratio, and VO
F3474 − 20
max), NIRS, joint/spinal stresses (biomechanics), skin inter- (RPE), rating of pain, soreness, discomfort, or comfort, or
face (shear, pressure, friction, and thermal), functional combinations thereof).
completion/effectivity tasks, completion times, and duration/
4.3 Functional Movement:
frequency of maintaining the posture. Subjective measures as
4.3.1 Posture Transitions—Posture transitions includes the
the user performs the task are psychophysical and psycho-
entire body with respect to user movements from prone to
physiological metrics (RPE, rating of pain, soreness,
supine, supine to prone, prone or supine to sitting, prone or
discomfort, or comfort, or combinations thereof).Additionally,
supine to a kneel, sitting to kneeling, sit to stand, kneel to
military and law enforcement should consider weapons and
stand, or some combination of these postures. This task’s
armor.
context involves dynamic changes of multiple joint angles and
4.2.9 Sideways Lunge—A sideways lunge involves the en-
center of gravity as the user transitions between postures.
tire body. The foot position is one foot beside the other at
Assessments of posture transitions can be conducted in a
greater than shoulder length apart (staggered). Assessments of
laboratory or field environment associated with industrial,
a sideway lunge can be conducted in a laboratory or field
military, medical (patient centric), first responder, and recre-
environment associated with industrial, military, medical, first
ationaldomains.Objectivemeasuresarebloodpressure,blood-
responder, and recreational domains. Objective measures are
oxygen saturation, range of motion, binary task completion,
range of motion, binary task completion, 3D volumetric
muscle activation/fatigue (EMG, integrated muscle activity,
changes of body segments/limbs, muscle activation/fatigue
time of muscle activity onset, frequency component analysis,
(EMG, integrated muscle activity, time of muscle activity
muscle synergies, or co-contraction, or combinations thereof),
onset, frequency component analysis, muscle synergies, or
NIRS, heart rate, heart rate variability, joint/spinal stresses
co-contraction, or combinations thereof), metabolic/energy
(biomechanics), skin interface (shear, pressure, friction, and
cost (rate of oxygen consumption, kilocalories expended, cost
thermal), functional completion/effectivity tasks, postural
of transport, heart rate, heart rate variability, respiratory ex-
stability, and completion time. Subjective measures as the user
change ratio, and VO max), NIRS, joint/spinal stresses
performs the task are psychophysical and psychophysiological
(biomechanics), skin interface (shear, pressure, friction, and
metrics (RPE, rating of pain, soreness, discomfort, or comfort,
thermal), functional completion/effectivity tasks, completion
or combinations thereof). Additionally, military and law en-
times, and duration/frequency of maintaining the posture.
forcement should consider weapons and armor. Lastly, all
Subjective measures as the user performs the task are psycho-
domains are concerned with quality of movement.
physical and psychophysiological metrics (rate of perceived
4.3.2 Hand Grip—Hand grip encompasses only the upper
exertion (RPE), rating of pain, soreness, discomfort, or
body unless grip is being assessed in conjunction with a task
comfort, or combinations thereof). Additionally, military and
that also involves the trunk/torso and lower body. This task’s
law enforcement should consider weapons and armor.
context involves varying postures of the hand. Assessments of
4.2.9.1 Hip Mobility—Hipmobilitymainlyencompassesthe
handgripcanbeconductedinalaboratoryorfieldenvironment
lower body and the trunk/torso. The hip is a very mobile joint.
associated with industrial, military, medical (patient centric),
Whenhipmobilityistestedwhiletheuserperformsataskwith
first responder, and recreational domains. Objective measures
the upper body, the upper body may also be of interest. This
are duration of maintaining the posture, ability to obtain the
task’s context is moving forward (flexion), backwards
posture, heart rate, heart rate variability, muscle activation/
(extension), sideways (abduction and adduction), and rotating
fatigue (EMG, integrated muscle activity, time of muscle
(internally and externally) at the hip. Internal and external activity onset, frequency component analysis, muscle
rotation can be completed with the hip maintained in any range
synergies, or co-contraction, or combinations thereof), NIRS,
of motion. Finally, the evaluation can integrate horizontal functional completion/effectivity tasks, joint stresses
abduction, horizontal adduction, or circumduction. Assess- (biomechanics), binary fit changes, skin interface (shear,
ments of hip mobility can be conducted in a laboratory or field pressure, friction, and thermal), 3D volumetric changes of
body segments/limbs, pressure points, and strength evaluation.
environment associated with industrial, military, medical, first
responder, and recreational domains. Objective measures are Subjective measures as the user performs the task are psycho-
physical and psychophysiological metrics (RPE, rating of pain,
range of motion, binary task completion, 3D volumetric
changes of body segments/limbs, muscle activation/fatigue soreness, discomfort, or comfort, or combinations thereof).
Additionally, military and law enforcement should consider
(EMG, integrated muscle activity, time of muscle activity
onset, frequency component analysis, muscle synergies, or weapons and armor.
co-contraction, or combinations thereof), metabolic/energy
4.3.3 Walk—Walk encompasses the entire body. This task’s
cost (rate of oxygen consumption, kilocalories expended, cost context involves terrain of varying slope: level, cross slopes,
of transport, heart rate, heart rate variability, respiratory ex-
incline, and decline. Further, walking direction (forward,
change ratio, and VO max), NIRS, joint/spinal stresses backward, sidestepping, and combinations of directions) is
(biomechanics), skin interface (shear, pressure, friction, and
relevant. Lastly, different types of environments such as over
thermal), functional completion/effectivity tasks, and duration/ ground, treadmill, rock, gravel, sand, snow, ice, and water
frequency of maintaining the posture, postural stability, and
should be considered. Assessments of walking can be con-
postural recovery (returning back to neutral posture). Subjec- ducted in a laboratory or field environment associated with
tive measures as the user performs the task are psychophysical industrial, military, medical (patient centric), first responder,
and psychophysiological metrics (rate of perceived exertion and recreational domains. Objective measures are blood
F3474 − 20
pressure, blood-oxygen saturation, time to completion, task ity of hit, probability of lethal hit, recoil time, aiming time,
kinematics (max/min joint angles, range of motion, and joint weapon stability (horizontal, vertical, and overall), body
angular velocity), kinetics (peak ground reaction forces, load- stability, postural stability, trigger control, time between shots,
ing rates, joint moments, joint reaction forces, joint contact mean target acquisition time, total target acquisition time,
forces, and joint powers), spatiotemporal gait metrics (pace, engagement time, ammunition reload, and total scenario
gait speed, cadence, stride length, step length, step height, step completion time. Many of the physical, physiological,
width, step width variability, double-limb support time, single- psychophysical, and psychophysiological metrics covered in
limbsupporttime,stance/swingratio,toeclearance,footcenter this practice for other tasks may also apply.
of pressure, left/right balance, and distance), gait efficiency,
4.3.6 Step Up/Down/Over Stairs or Obstacles—Step up/
power, metabolic/energy cost (rate of oxygen consumption,
down/over stairs or obstacles encompasses the entire body.
kilocalories expended, cost of transport, heart rate, heart rate
Assessments of step up/down/over stairs or obstacles can be
variability, respiratory exchange ratio, and VO max), NIRS,
2 conducted in a laboratory or field environment associated with
skin interface (shear, pressure, friction, and thermal), 3D
industrial, military, medical (patient centric), first responder,
volumetric changes of body segments/limbs, and muscle ac-
and recreational domains. Objective measures are blood
tivityandfunction(peakEMG,integratedmuscleactivity,time
pressure, blood-oxygen saturation, postural stability metrics
of muscle activity onset, frequency component analysis,
(variability of ground reaction forces, center of pressure
muscle synergies, or co-contraction, or combinations thereof).
deviations and path length, limits of stability, and dynamic
Subjective measures as the user performs the task are psycho-
postural stability index) time to completion, task kinematics
physical and psychophysiological metrics (RPE, rating of pain,
(max/min joint angles, range of motion, and joint angular
soreness, discomfort, or comfort, or combinations thereof).
velocity), kinetics (peak ground reaction forces, loading rates,
4.3.4 Run—Run encompasses the entire body. This task’s joint moments, joint reaction forces, joint contact forces, and
context involves terrain of varying slope: level, cross slopes, joint powers), spatiotemporal gait metrics (pace, gait speed,
incline, and decline. Further, running direction (forward, cadence, stride length, step length, step height, step width, step
backward, sidestepping, and combinations of directions) is width variability, double-limb support time, single-limb sup-
relevant. Lastly, different types of environments such as over port time, stance/swing ratio, toe clearance, foot center of
ground, treadmill, rock, gravel, sand, snow, ice, and water pressure, left/right balance, and distance), gait efficiency,
should be considered. Assessments of a run can be conducted power, metabolic/energy cost (rate of oxygen consumption,
in a laboratory or field environment (depending on equipment) kilocalories expended, cost of transport, heart rate, heart rate
associatedwiththeindustrial,military,medical,firstresponder, variability, respiratory exchange ratio, and VO max), NIRS,
and recreational domains. Objective measures are blood skin interface (shear, pressure, friction, and thermal), 3D
pressure, blood-oxygen saturation, time to completion, task volumetric changes of body segments/limbs, and muscle ac-
kinematics (max/min joint angles, range of motion, and joint tivityandfunction(peakEMG,integratedmuscleactivity,time
angular velocity), kinetics (peak ground reaction forces, load- of muscle activity onset, frequency component analysis,
ing rates, joint moments, joint reaction forces, joint contact muscle synergies, or co-contraction, or combinations thereof).
forces, and joint powers), spatiotemporal gait metrics (pace, Subjective measures as the user performs the task are psycho-
gait speed, cadence, stride length, step length, step height, step
physical and psychophysiological metrics (RPE, rating of pain,
width, step width variability, double-limb support time, single- soreness, discomfort, and comfort).
limbsupporttime,stance/swingratio,toeclearance,footcenter
4.3.7 Ladder Ascent or Descent—Entails physically climb-
of pressure, left/right balance, and distance), gait efficiency,
ing rungs with hands and feet with or without fall protection.
power, metabolic/energy cost (rate of oxygen consumption,
Ladder ascent or descent is applicable to the entire body.
kilocalories expended, cost of transport, heart rate, heart rate
Assessments of ladder ascent or descent can be conducted in a
variability, respiratory exchange ratio, and VO max), NIRS,
2 laboratory or field environment associated with industrial,
skin interface (shear, pressure, friction, and thermal), 3D
military, first responder, or recreational domains. Objective
volumetric changes of body segments/limbs, functional
measures are time to complete task, postural stability metrics
completion/effectivity/accuracy/precision weapons and armor,
(variability of ground reaction force (GRF), center of pressure
posturalstability,andmuscleactivityandfunction(peakEMG,
(COP) deviations and path length, limits of stability, and
integrated muscle activity, time of muscle activity onset,
dynamic postural stability index), kinematic metrics (joint
frequency component analysis, muscle synergies, or co-
angles, range of motion, and joint angular velocity), kinetics
contraction, or combinations thereof). Subjective measures as
(peak ground reaction forces, joint moments, joint reaction
the user performs the task are psychophysical and psycho-
forces, joint contact forces, and joint powers), muscle activity
physiological metrics (RPE, rating of pain, soreness,
and function (peak EMG, integrated muscle activity, time of
discomfort, or comfort, or combinations thereof).
muscle activity onset, frequency component analysis, muscle
4.3.5 Marksmanship—Marksmanship includes the entire synergies, or co-contraction, or combinations thereof),
body. This task’s context involves both static and dynamic metabolic/energy cost (rate of oxygen consumption, kilocalo-
activities.Assessments of marksmanship can be conducted in a ries expended, cost of transport, heart rate, heart rate
laboratory (simulated) or field (live-fire) environment associ- variability, respiratory exchange ratio, and VO max), NIRS,
ated with the military (and first responder: law enforcement) andcapabilityofperformingthetask(forexample,threepoints
domain. Objective measures are precision, accuracy, probabil- of contact, materiel, and body armor (only for military or law
F3474 − 20
enforcement applications)). Subjective measures as the user task completion (yes/no) in military applications), and
performs the task are psychophysical and psychophysiological subjective/qualitative feedback in military applications.
metrics (RPE, rating of pain, soreness, discomfort, or comfort,
4.3.10 Crawl—Low and high crawling are applicable to the
or combinations thereof).
entire body. Assessments of a crawl can be conducted in a
laboratory or field environment associated with industrial,
4.3.8 Utility Pole, Tree, or Other Non-Rung-Based Ascent
military, medical, first responder, and recreational domains.
or Descent—Using gear such as straps, ropes, webbing, pulley
Objectivemeasuresaretimetocompletetask,posturalstability
systems, anchors, ratchets, belay devices, or other specialized
metrics (variability of GRF, COP deviations and path length,
equipment and footwear, or combinations thereof, to climb.
limits of stability, and dynamic postural stability index),
This section is applicable to the entire body. Assessments can
kinematic metrics (joint angles, range of motion, and joint
be conducted in a laboratory or field environment associated
angular velocity), kinetics (peak ground reaction forces, joint
with industrial, military, first responder, and recreational do-
moments, joint reaction forces, joint contact forces, and joint
mains. Objective measures are time to complete task, postural
powers), mu
...



Questions, Comments and Discussion
Ask us and Technical Secretary will try to provide an answer. You can facilitate discussion about the standard in here.
Loading comments...